Due to a variety of conditions (e.g. trauma, missing teeth, infection, tumor removal) the bones of the face lack sufficient quantity and quality to support proper facial contours, or support for placement of dental implants. Over time, aging, osteoporosis and stress can also add to bone loss. Bone can be replaced by a variety of techniques, depending on the type of deficit involved, and future plans to restore functionality and esthetic appearance.
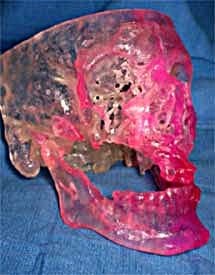
Natural Vs. Artificial Bone Grafting
It is always best if possible to restore missing bone with the patient's own natural bone. Many small defects can be repaired by obtaining bone from locations within the oral cavity, mostly from the lower jaw. Larger defects require areas that will supply a larger quantity of bone. We commonly utilize the knee cap (tibia), hip bone or outer layer of the skull for this purpose.
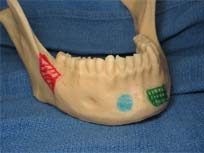
Depending on the shape of the defect involved, either block or particle shaped bone will be required.
Bone grafts taken from within the mouth are normally done in office, usually under sedation. The bone taken eventually regenerates, leaving the jaw as strong as prior to the bone graft.
Bone taken from the knee (tibia) can also be performed in our state-of-the-art, office-based, outpatient surgical facility under strict sterile conditions. Patients leave the office without the need of assistance with walking, and can return to normal activities within a few weeks. Bone grafts taken from the hip bone require surgery to be performed in the hospital, normally with an overnight stay. Following normal healing, our patients return to normal activities within a few weeks following surgery.
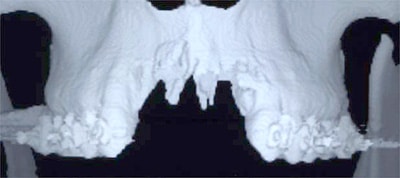
Determining the exact amount , shape and placement of the bone is based on an examination, models, and a 3 dimensional Cone Beam CT scan of the areas involved. Special cases require the manufacture of a custom anatomical model of the facial bones in order to plan your surgery.


Some cases may allow for the use of artificial bone to be used as a substitute, or in conjunction with natural bone. This bone can come from a variety of sources (animal, coral, algae, synthetic), or may be freeze dried (harvested from a cadaver). Be assured that freeze dried bone is thoroughly tested and prepared to remove any harmful materials before its use in humans. Recently, a new form of genetically engineered bone (rBMP/Infuse?) has been introduced that eliminates the need for bone harvesting, or the need for bone substitutes. Incorporation time of the graft varies from 3-9 months, depending on the situation. Many times, dental implants can be placed at the same time as the bone graft.
The Following Is A Short Discussion Of The Most Common Techniques Used In Bone Grafting Surgery:
Sinus Lift Procedure
The upper jaw (maxilla) has two open cavities, called the sinuses. These cavities, above the posterior teeth, normally act to filter and moisturize the air we breathe. After tooth loss, bone can be lost resulting in a relatively enlarged sinus cavity.
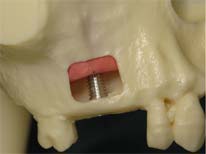
When dental implants are considered in this area of limited bone, surgery is performed to rebuild bone, allowing implants to be placed. Through an small incision, the lining of the sinus cavity is exposed and elevated. Bone grafts and implants can then be placed. This can be done in a single stage or in multiple procedures, depending on your condition.
Once the bone graft and implants have healed, permanent teeth can be placed by your dentist. The average treatment time can be from 4-12 months.
Ridge-Augmentation
In cases where either bone height and/or width are deficient, an onlay graft is normally required in preparation for implant placement. Small to medium sized defects can be restored with a graft taken from the lower jaw while larger areas may need to be grafted with bone taken from the hip.
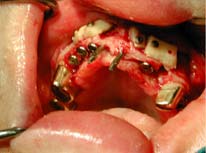
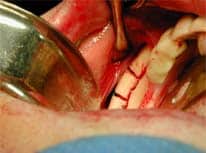
Depending upon your condition, surgery may need to be done in one or more stages.
Nerve-Repositioning
The inferior alveolar nerve, which gives feeling to the lower lip and chin, may need to be moved in order to make room for placement of dental implants to the lower jaw.
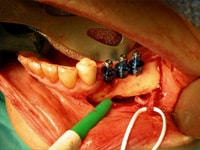
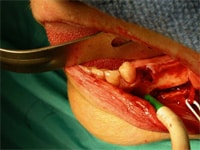
This procedure is limited to the lower jaw and indicated when teeth are missing in the area of the two back molars and/or and 2nd premolar, with the above-mentioned secondary condition. Since this procedure is considered a very aggressive approach (there is almost always some postoperative numbness of the lower lip and jaw area, which dissipates only very slowly, if ever), usually other options are considered first such as building the ridge up with an onlay bone graft, a tent pole graft, or expanding the bone through a process called distraction osteogenesis.
Distraction Osteogenesis
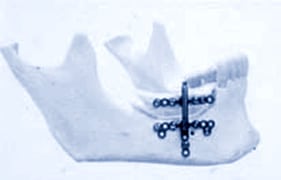
A predictable alternative to the placement of onlay grafts is to grow bone by distraction. This technique is similar in principle to the orthopedic principles of limb lengthening. In the area of bone defect, an appliance is placed in the area of needed bone. Over a period of approximately 2 weeks, old bone is stretched apart and new bone grows in its place. After this new bone heals (~3 months), dental implants can be placed.
Platelet Rich Plasma
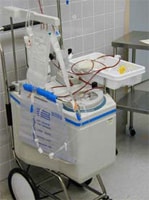
The use of Platelet Rich Plasma (PRP) has been developed in order to enhance the body?s healing capacity in a variety of situations. With respect to it?s use in bone grafting, PRP dramatically improves not only the quality and quantity of bone healing, but also the speed at which the bone graft heals, while reducing postoperative discomfort associated with the procedure.
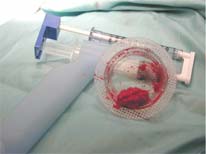
During the bone graft procedure, a small test tube of blood is withdrawn from a vein in the arm. This blood is prepared in a special device that separates the platelets from the body of the blood. By adding chemicals to release the platelet's special growth factors (proteins), the PRP is added to the graft to enhance healing.
PRP has many clinical applications:
- Bone grafting for dental implants. This includes onlay and inlay grafts, sinus lift procedures, ridge augmentation procedures, and closure of cleft, lip and palate defects.
- Repair of bone defects creating by removal of teeth or small cysts.
- Repair of openings between the sinus cavity and mouth.
Read What Our Patients Have To Say!
Frequently Asked Questions About PRP
Yes. During the outpatient surgical procedure a small amount of your own blood is drawn out via the IV. This blood is then placed in the PRP centrifuge machine and spun down. In less than fifteen minutes, the PRP is formed and ready to use.
Not always. In some cases, there is no need for PRP. However, in the majority of cases, application of PRP to the graft will increase the final amount of bone present in addition to making the wound heal faster and more efficiently.
Unfortunately not. The cost of the PRP application (approximately $500-750) is paid by the patient.
No. PRP must be mixed with either the patient's own bone, a bone substitute material such as demineralized freeze-dried bone, or a synthetic bone product.
Very few. Obviously, patients with bleeding disorders or hematologic diseases do not qualify for this in-office procedure. Check with Dr. Sultan to determine if PRP is right for you.
Depending on the patient’s overall health and the extenbt of the procedure, the total recovery time for bone grafting can vary from patient to patient. Usually the recovery process entials immobilization, pain medication, follow-up appointments, and rehabilitation.
Typically, it’s advised to wait at least four months before looking into getting a dental implant for an area that has undergone bone grafting. That’s about how long it takes before the area will be strong enough to support an implant.
There are no food restrictions after getting a bone graft. It is advised to do your best to chew your food on the opposite side of the mouth that you had your bone grafting done on.
The main reason a bone graft can fail is from infection. Believe it or not, our mouths are one of the dirtiest places on our body. So infection can occur if post-operative instructions aren’t followed closely.
Schedule A Consultation With Dr. Sultan!
Take advantage of Dr. Sultan's extensive experience and renowned medical skills. Book a personalized consultation at our Fort Lauderdale office by calling (954) 771-8772 or by clicking here to send us an email message form. We look forward to serving you!